Team:TU-Delft/HP
From 2012.igem.org


Snifferomyces - A Tuberculosis Screening Automaton
What is the use of technology, if it cannot contribute to improving human life? With this thought in mind, the TU Delft 2012 iGEM team, composed of students from the life sciences, bioinformatics, applied physics, aerospace, maritime, mechanical and chemical engineering disciplines decided to use the platform of synthetic biology, addressing a real challenge affecting millions of people .
Inspired by the sniffer rats trained to smell the presence of tuberculosis, the team decided to build an autonomous olfactory system to detect volatile compounds, by re-inventing man's oldest industrial microorganism, yeast, to provide for a non-invasive, rapid and cost-effective diagnosis system for tuberculosis. The reason why we have chosen for yeast, is that yeast is relative cheap to grow. Furthermore yeast has the ability to sense low amounts of concentration of specific compounds and can be storage for a long time.
For our Human Practice we did a study in to what extent our proof of principle, if it would be translated into a product, could make a difference. To answer this we evaluate the most important parts of this question below.
What is Tuberculosis?
Tuberculosis is a bacterial infection. TB usually attacks the lungs, but can also attack other parts of the body, such as the brain, spine, or kidneys. TB bacteria can live in the body without making a person sick. This is called latent TB infection. People with latent TB infection do not feel sick, do not have TB symptoms, and cannot spread TB bacteria to others. Some people with latent TB infection go on to develop TB disease.
TB becomes even a larger problem because of HIV, 60.1% of TB patients tested for HIV were HIV-positive. HIV-patients with TB have to be cured even faster because of their immune system is weakened.
In 2010, 8.8 million people were infected with TB and 1.4 million died from it. Over 95% of TB deaths occur in low -and middle- income countries.
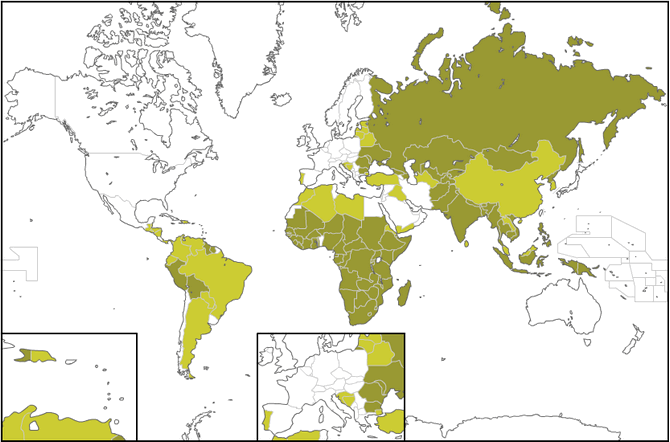
At the map below you can see the countries suffering from Tuberculosis. According to www.vaccinatiesopreis.nl the dark green refers to many cases of TB, the light green to less and the white to a few cases.
The problem
The problem of tuberculosis lies mainly in the less developed countries. The frontline are the remote areas where the people have no or limited access to hospitals with sufficient facilities. Standard TB diagnostic tools are either expensive and need to be used in a lab setting or are not very reliable, all these reasons are posing major barriers for diagnosing.
Six Ways to Diagnose Tuberculosis
These are six main diagnosis tools for TB. The problem is that there is not one of them that is very reliable and also suitable for the frontline. Not suitable for the frontline because it needs facilities, doesn't give a quick result and/or is expensive.
- Tuberculin Skin Test (TST)
- Sputum Smear Microscopy (SSM)
- Polymerase Chain Reaction (PCR)
- Blood Test for TB detection
- Chest X-ray
- Culture
Our ideal Solution
A cheap test that quickly gives an reliable result, that can be taken by a 4x4 car to the people.
What would a test based on our principle contribute?
Reach
Yeast cells can be kept in dried form, which makes them very well transportable and easy to store. Remote areas can be easily reached.Evaluating of test result
Now we did the tests with GFP but if would use a visible output, it would be very easy to see a result. Which also mean that there are not many facilities needed.Cheap
The producing of a large amount of yeast cells is in general not this expensive.Reliability
This is something that should still be evaluated.Waiting time
The waiting time for the result will be approximately 3 hours.Conclusion
We strongly believe that our project is well worth to be further developed. We believe it can make a change in how diagnostics in remote areas take place. But also for areas with facilities, it can be a cheap alternative for the diagnosing of other diseases that can be detected by specific compounds.
Example Mozambique; lack of facilities
Mozambique ranks the 19th among the 22 Tuberculosis High Burden Countries 2011 according to the WHO.One of our team members, Isabelle, traveled to Mozambique in july 2011. The lack of the diagnostic capacity is very clear at the hospital of Ilha de Mocambique. Ilha de Mocambique inhabits 14.000 people and they are relying on the hospital there. This picture of the Hospital is taken in july 2011. In contrary to what Wikipedia states, part of this building is still being used as a hospital.

Possible applications of the Sniffer-O-Meter!
The Royal Dutch Military Police regarding a detector of explosives.
Every day, 1800 member of the Royal Dutch Military Police are present at Schiphol to detect possible threats to the National Security. One part of their job is to be on the lookout for explosives. This is where smell plays an important part! Explosives are usually detected by Explo-dogs, dogs which have been trained to detect the scent associated with explosives.

An Explo-Dog is being trained to detect 14 different types of smells, which for security reasons will not be mentioned, in different combinations. The largest amount of explosives are covered by this intensive training after which they will work together with a canine trainer of the Military Police, such as Rick van Vulpen who spoke to us on this matter.
A Sniffer-O-Meter could be made to smell these same 14 volatiles and to give a signal dependent on what combination of volatiles is detected. The Snifferomyces is designed to be a general platform for any possible smell, smelling explosives is only one of the possible applications. The Sniffer-O-Meter could be redesigned to be carried around or to stay at a central position, like a fire detector.
"Micro-organisms and GMOs would definitely be used if it would improve the National Security."
The most important feature should be a very low number of false positives. It is a waste when the team responds to a false alarm, this costs a lot of time and money. Genetic modification is a new, important technology which, when whithin certain safety standards should definitely be used. At the moment we are experimenting with a chemical 'Nose', but this technology also responds to coca-cola, which has caused a lot of false alarms. In the lab a small error rate might be seen as acceptable, but in the field this is less so.
On the job, dog and trainer work together as coworkers. And even though canine is trained to smell, his secundary role is to give a secure feeling to the crowd at an airport and the trainer. Of course this role would never be replaced by micro-organisms, although they could prove to become a solid addition to the general equipment.
We would like to thank Rick van Vulpen for a nice chat on this subject!
The picture is from "Safety and Security", October 2012, a supplement of the Telegraaf.
Talk with Dr. Lutter about the applicability of our research within the medical field
To get a better overview of what the medical field would think of our research, we talk to Dr. Rene Lutter ( is doing research at the functioning of granuloma in tuberculosis and if you can read the functioning of granuloma from the parameters in breath-condensate, at the Academic Medical Center (AMC), University of Amsterdam, the Netherlands.
Has we explained our project to this doctor he became very enthusiastic about the many possibilities one can do with it. Of course plenty more research is needed before one can actually use this in the medical field, but the beginning of our project will probably eventually lead up to a new detection method in the medical field. He gave a couple of examples that would be improved with this new detection method, those are listed below.
Intensive care
There are people coming to the intensive care with an unknown infection which can be deadly if not treated on time. Now a days doctors first need a sample of the infection, let the bacteria grow and identify it, and treat the patient with the right medicine. This whole process cost a lot of time, which some patients do not have unfortunately. If we would have a broad platform of detection many different gaseous compounds, the diagnosing of the unknown infections would be a lot faster and more people would cured.
Resistant TB
There are several types of resistant TB, which means that the medicine will not cure the TB from the patient. A patient gets resistant TB either from taking their medication wrong or directly from another resistant TB patient. Diagnosing if a patient has resistant TB takes approximately 2 to 3 months. With the upcoming technology one would be able to detect different compounds of a resistant TB, and one would find out quickly if someone is suffering from a resistant TB and would get the appropriate treatment faster.
HIV and TB
People who are infected with HIV have a disoriented immune system. This will give the opportunity for other infections to easily enter the human body. TB bacteria become active if the immune system cannot stop this from growing. So the combination of those two diseases is in many cases deadly if not diagnosed and treated.
Fact: From the 8.8 million people who got TB in 2010, there were 1.1 million also HIV-positive.82% of those people live in the Sub-Saharan Africa. From all the aids patients who die, half of them die from TB.
[http://www.artsenzondergrenzen.nl/over-ons/dossiers/medische-dossiers/dossier-tuberculose/tuberculose-en-hiv-aids.aspx]
Diagnosing TB by patients with saliva-test or even by x-ray photos who are seropositive is not always giving the correct diagnosis. So in order to treat these patients a better and faster diagnose of TB is necessary. So by able to detect compounds of TB, no matter the patient’s own condition, a proper diagnose can be made and more people would be treated in much earlier state.
To conclude, our research has many possibilities within the medical field. So hopefully in the near future this wills safe many people.
We would like to thank Dr. Rene Lutter for his input in our project!

To get a better overview of what the medical field would think of our research, we talk to Dr. Rene Lutter ( is doing research at the functioning of granuloma in tuberculosis and if you can read the functioning of granuloma from the parameters in breath-condensate, at the Academic Medical Center (AMC), University of Amsterdam, the Netherlands.
Has we explained our project to this doctor he became very enthusiastic about the many possibilities one can do with it. Of course plenty more research is needed before one can actually use this in the medical field, but the beginning of our project will probably eventually lead up to a new detection method in the medical field. He gave a couple of examples that would be improved with this new detection method, those are listed below.
Intensive care
There are people coming to the intensive care with an unknown infection which can be deadly if not treated on time. Now a days doctors first need a sample of the infection, let the bacteria grow and identify it, and treat the patient with the right medicine. This whole process cost a lot of time, which some patients do not have unfortunately. If we would have a broad platform of detection many different gaseous compounds, the diagnosing of the unknown infections would be a lot faster and more people would cured.
Resistant TB
There are several types of resistant TB, which means that the medicine will not cure the TB from the patient. A patient gets resistant TB either from taking their medication wrong or directly from another resistant TB patient. Diagnosing if a patient has resistant TB takes approximately 2 to 3 months. With the upcoming technology one would be able to detect different compounds of a resistant TB, and one would find out quickly if someone is suffering from a resistant TB and would get the appropriate treatment faster.
HIV and TB
People who are infected with HIV have a disoriented immune system. This will give the opportunity for other infections to easily enter the human body. TB bacteria become active if the immune system cannot stop this from growing. So the combination of those two diseases is in many cases deadly if not diagnosed and treated.
Fact: From the 8.8 million people who got TB in 2010, there were 1.1 million also HIV-positive.82% of those people live in the Sub-Saharan Africa. From all the aids patients who die, half of them die from TB.
[http://www.artsenzondergrenzen.nl/over-ons/dossiers/medische-dossiers/dossier-tuberculose/tuberculose-en-hiv-aids.aspx]
Diagnosing TB by patients with saliva-test or even by x-ray photos who are seropositive is not always giving the correct diagnosis. So in order to treat these patients a better and faster diagnose of TB is necessary. So by able to detect compounds of TB, no matter the patient’s own condition, a proper diagnose can be made and more people would be treated in much earlier state.
To conclude, our research has many possibilities within the medical field. So hopefully in the near future this wills safe many people.
We would like to thank Dr. Rene Lutter for his input in our project!

 "
"